Patient Outcome
From Painful Sensitivity to a Healthy, Confident Smile
Ashley was referred by her pediatric dentist for relief from gum sensitivity and irritation she had been experiencing.
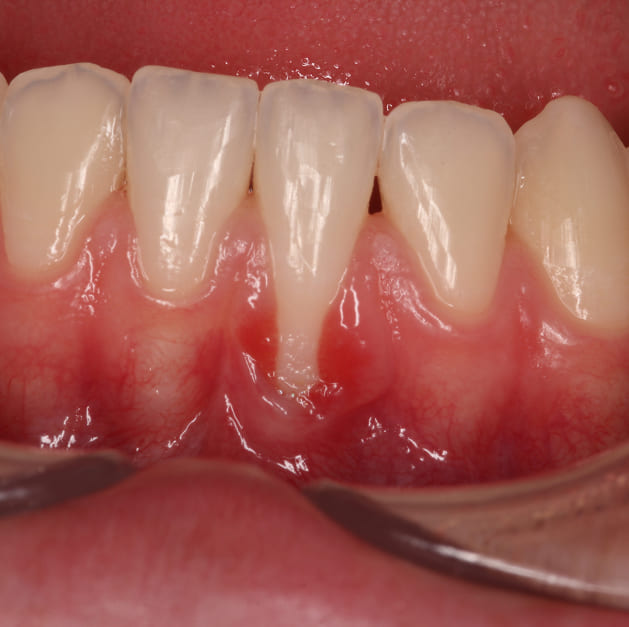
Before
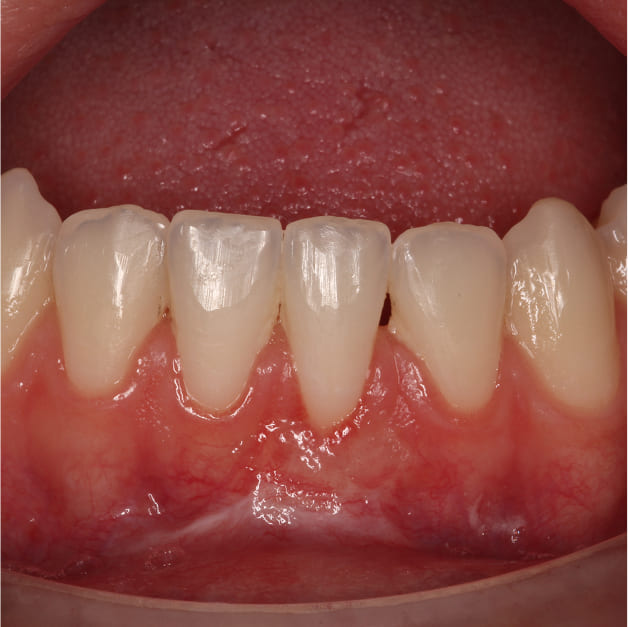
After
Patient
Ashley
Surgeon
Dr. Stephen Hutton
Recovery
4-6 weeks
"I used to dread eating ice cream or drinking cold water because it would hurt so much. Now I do not even think about it. My gums look and feel completely normal."
Ashley was 19 when her pediatric dentist referred her after two years of persistent gum sensitivity. Cold food, hot beverages, and brushing certain spots in her mouth triggered sharp, predictable pain that had become a daily inconvenience.
The source was localized recession on two lower front teeth. The root surfaces were visibly exposed on both, and the tissue around them was thin and continuing to break down. Despite her age, the recession had progressed far enough to warrant surgical correction — and early treatment was the best way to prevent it from becoming more complex.
Initial Condition & Evaluation
Ashley presented with Miller Class I recession on the mandibular central and lateral incisors on her left side, measuring approximately 3 millimeters. The exposed root surfaces were sensitive to touch and to temperature changes.
The surrounding tissue was thin and showed evidence of chronic irritation. A high frenal attachment was identified as a contributing factor, placing steady tension on the marginal gingiva and pulling it apically during normal lip movement.
Ashley's oral hygiene was otherwise good, but she had been brushing the affected area with more force than necessary — a common response to sensitivity that was inadvertently making the recession worse.
Contributing Factors in Young Patients
Gum recession in young patients often surprises families, who associate it with aging. But several factors can drive recession early.
- A thin gingival biotype — a genetic characteristic — makes the tissue more susceptible to recession from normal mechanical forces.
- An aberrant frenal attachment can pull the gingival margin away from the tooth surface with every lip movement.
- Aggressive brushing with a firm-bristled brush is among the most common causes of recession in otherwise healthy young patients.
- In some cases, orthodontic treatment contributes to recession when teeth are moved to the edge of or outside the alveolar bone envelope.
Treatment Plan
A two-component approach was recommended: a frenectomy to release the frenal tension on the marginal tissue, combined with a connective tissue graft to restore root coverage and build tissue thickness over the exposed areas.
Both components would be completed in a single appointment. Addressing the underlying cause and the resulting defect simultaneously gives the most stable long-term outcome — correcting only one without the other risks early recurrence.
Ashley and her parents were also walked through proper brushing technique — specifically, switching to a soft-bristled brush and using gentle circular motions rather than horizontal scrubbing. That habit change was just as important to the lasting result as the surgery itself.
Procedure & Recovery
The frenectomy was performed first to release the tissue pull that had been contributing to the recession. A connective tissue graft was then harvested from the palate and placed beneath a coronally advanced flap over the exposed root surfaces.
The procedure was well-tolerated under local anesthesia. Ashley reported only mild tenderness at the palatal donor site, which resolved within five days.
At the two-week follow-up, early tissue healing looked excellent. By six weeks, the graft had matured, the roots were fully covered, and the gingival margin had stabilized at the correct anatomic position.
Outcome
Ashley's sensitivity resolved completely. The newly established tissue created a thick, protective barrier over the root surfaces, and the frenectomy eliminated the mechanical force that had been driving the recession in the first place.
The result was also aesthetically natural. The tissue blended with the adjacent gingiva in color, texture, and contour — there was nothing visible to suggest surgery had been performed.
At her six-month follow-up, the tissue remained stable with no signs of recurrence. Ashley had maintained her brushing habit changes and excellent oral hygiene. The sensitivity she had lived with for two years was gone, and she reported feeling comfortable smiling without hesitation for the first time in a long time.
Clinical Notes
This case underscores the importance of early referral for recession in young patients. When identified and treated promptly, recession can be corrected with highly predictable outcomes before significant root damage or bone loss occurs.
Addressing the etiology of recession, in this case the frenal pull and brushing trauma, is as important as the surgical correction itself. Without eliminating the causative factors, grafted tissue is at risk of receding again.
- Combining frenectomy with connective tissue grafting in a single procedure addressed both the cause and the defect simultaneously.
- Patient education on atraumatic brushing technique was essential for long-term stability of the surgical result.
- Early intervention in young patients with thin biotype and recession can prevent progression to more complex defects that are harder to treat predictably.
Your Story Starts Here
Ready to See What's Possible?
Request a consultation and let our specialists evaluate your situation. Clear options, honest answers, no pressure.