Patient Outcome
Severely Exposed, Demineralized Roots Restored in a Single Microsurgical Visit
Niko had longstanding gum recession with severe root exposure affecting multiple teeth.
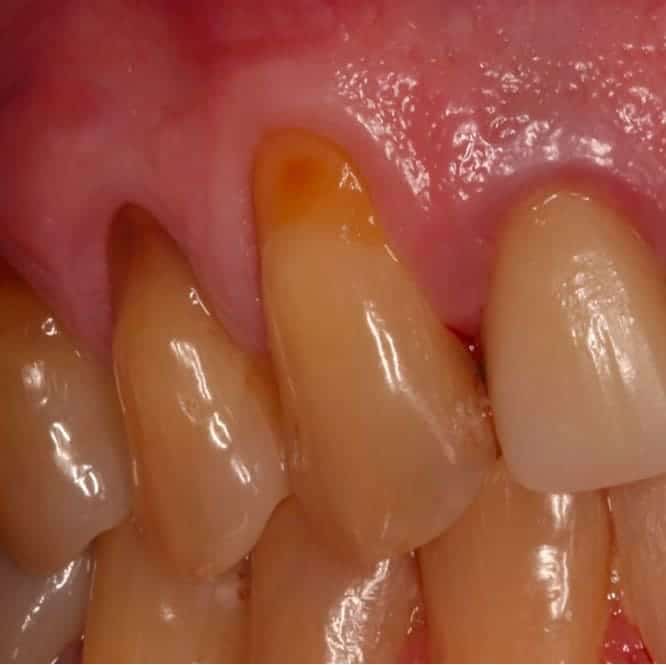
Before
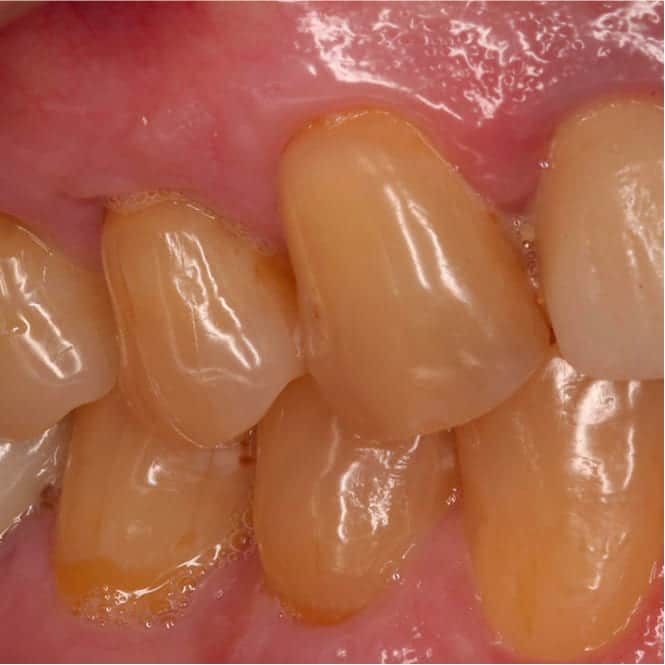
After
Patient
Niko
Surgeon
Dr. Stephen Hutton
Recovery
6-8 weeks
"I had been told by another dentist that my roots were too far gone and there was nothing that could be done. Dr. Hutton not only fixed them, he made them look better than I ever expected."
Niko had watched his gums recede gradually over almost a decade. What began as mild sensitivity to cold had progressed to visible root exposure, discoloration, and constant discomfort across several teeth on his upper left side.
By the time he sought treatment, the roots weren't just exposed — they had become demineralized from years of unprotected contact with the oral environment. His general dentist referred him for a microsurgical root coverage consultation after determining the case was beyond standard treatment approaches.
Initial Condition & Diagnosis
Niko presented with Miller Class II and Class III recession affecting the upper left premolars and canine, with recession depths ranging from 4 to 6 millimeters. The exposed root surfaces were discolored, rough to probing, and showed visible signs of surface demineralization.
The surrounding tissue was thin and fragile — a biotype that predisposes patients to progressive recession without intervention. A high frenal attachment was also identified, placing additional tension on the marginal tissue.
Niko had avoided chewing on the affected side entirely. The thermal sensitivity was consistent and significant, and the exposed roots had become a source of daily discomfort.
Why This Case Was Complex
Demineralized root surfaces create a specific challenge in coverage procedures because the altered surface chemistry and rough texture interfere with soft tissue attachment.
- Demineralized roots require careful surface preparation to create a biologically receptive base for the graft to attach to.
- The combination of severe recession depth and thin tissue biotype made conventional grafting techniques less predictable than in a straightforward case.
- Multiple adjacent teeth needed treatment simultaneously, requiring flap design that maintained sufficient blood supply across the entire surgical field.
Treatment Plan & Microsurgical Approach
A connective tissue graft procedure using microsurgical technique was planned. This involved harvesting a graft from the palate and placing it beneath a coronally advanced flap over the prepared root surfaces.
Before graft placement, the exposed root surfaces were meticulously debrided and treated with root biomodification agents to remove the demineralized layer and create a surface chemistry that supports new connective tissue attachment.
Microsurgical instruments and magnification were used throughout to minimize tissue trauma and achieve precise flap adaptation — both of which are especially important in complex multi-tooth recession cases where predictability depends on technique.
Procedure & Recovery
The procedure was completed in a single visit under local anesthesia. After root surface preparation, the connective tissue graft was secured over the exposed roots and the overlying flap was advanced coronally and sutured with microsurgical precision to achieve complete, tension-free coverage.
Niko received detailed postoperative instructions with emphasis on gentle oral hygiene and a soft diet during the initial healing window. He reported minimal discomfort, managed without prescription medication.
At four weeks, tissue color, thickness, and margin position were all tracking well. By eight weeks, the graft had fully integrated and the tissue was mature, stable, and noticeably thicker than what had been there before.
Outcome
Complete root coverage was achieved on all treated teeth. The sensitivity that had been a daily problem for Niko was gone.
The new tissue was significantly thicker than the original fragile biotype, providing a more resilient barrier against future recession. Gingival margins were at anatomically correct levels with a natural scalloped contour.
Niko reported that both his comfort and his confidence returned. He was eating normally again, no longer guarding the affected side, and no longer self-conscious about the appearance of his gums.
Clinical Notes
This case highlights the importance of root surface preparation in demineralized root coverage cases. Without thorough debridement and biomodification, the compromised root surface would likely have prevented predictable connective tissue attachment.
Microsurgical technique was instrumental in achieving complete coverage across multiple adjacent recession sites. The reduced tissue trauma associated with microsurgical flap management improved vascularity and graft survival.
- Root biomodification with citric acid or EDTA followed by enamel matrix derivative application improved the biological interface between the graft and the demineralized root surface.
- Connective tissue grafting simultaneously increased tissue thickness, reducing the likelihood of future recession recurrence.
- Simultaneous treatment of multiple adjacent sites under a single flap preserved the interproximal papillae and produced a more uniform esthetic result.
Your Story Starts Here
Ready to See What's Possible?
Request a consultation and let our specialists evaluate your situation. Clear options, honest answers, no pressure.